Diabetic Eye Disease
Diabetes: Too Much Sugar is No Eye Candy
Diabetes is an increasingly common disease in the United States. A recent alarming surge in the number of new diagnoses has doctors scrambling for answers. One culprit is the high-fat, high-sugar diet in our society that results in widespread obesity.
Diabetes is caused by a relative lack of or a resistance to insulin, an important hormone secreted by the pancreas to control the amount of sugar in the blood. Besides increasing the risk of heart attacks, strokes, kidney failure, nerve damage, and foot problems, diabetes is also detrimental to the eyes. It may affect vision in several ways, most notably by affecting the retina, a disease called diabetic retinopathy.
How Does Diabetes Cause Retina Problems?
The retina is analogous to the film of a camera; it is the sensory part of the eye that actually sees. Diabetes damages the small blood vessels in the retina, causing them to leak and bleed, leading to swelling of the retina. Eventually the blood vessels close off. The starved retina releases chemical signals that induce more blood vessels to grow. However, these new blood vessels are abnormal. They can lead to scarring, bleeding, and even detachment of the retina, all of which can cause loss of vision.
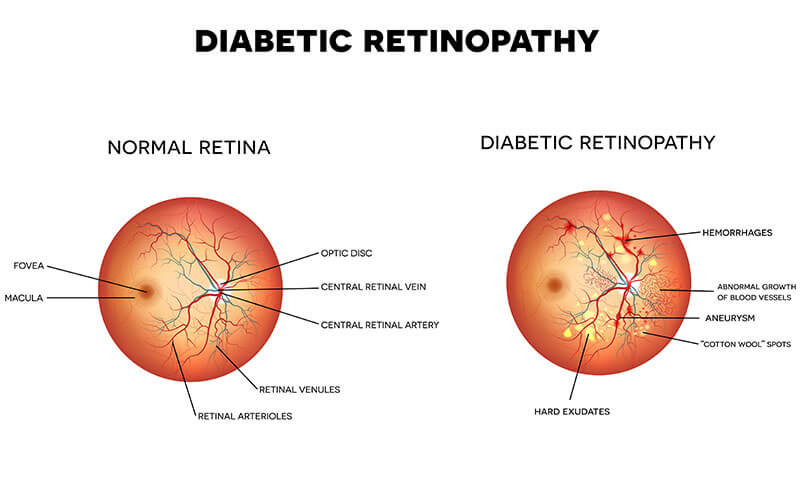
Symptoms of Diabetic Retinopathy
Until late in the disease, diabetic retinopathy usually has no symptoms. While some patients experience gradual blurring of vision, for others the problem goes undetected until one day the vision drops precipitously. Fortunately, because of increasing awareness of diabetic retinopathy among primary care physicians, many more patients are being referred to eye doctors for regular screening examinations. This has helped to prevent many devastating complications of diabetes in the eye.
Diagnosis
A dilated eye exam is essential to the diagnosis of diabetic retinopathy. The more severe the disease, the more frequent the follow-up visits need to be. Even a diabetic patient without eye disease is recommended to have an annual eye exam.
Treatment
The treatment of diabetic retinopathy depends on its severity. Early on, no treatment is necessary, but this does not mean that damage to the eye hasn’t already occurred. Once it has crossed a critical threshold, diabetic retinopathy may require treatment such as laser treatment, injections of medications into the eye, or even surgery. Not every patient will respond favorably to treatments. For some patients, the condition of their eyes continues to deteriorate, which is why prevention is imperative.
Once diabetes develops, some key measures will mitigate its damage. One of the most important steps is to control high blood pressure. If this is not done, the combination of diabetes and high blood pressure will exponentially increase the risk of irreversible harm to the heart, brain, kidneys, eyes, and other organs. Clinical studies have demonstrated the benefits of good diabetic control (keeping the blood sugar level as close to normal as possible). It is by far the best way to maintain your precious health and sight.
